PIDP 3210 Curriculum Development
Vancouver Community College
Kathryn Truant
November 13, 2016
Lesson Plan Rationale
Lesson #3
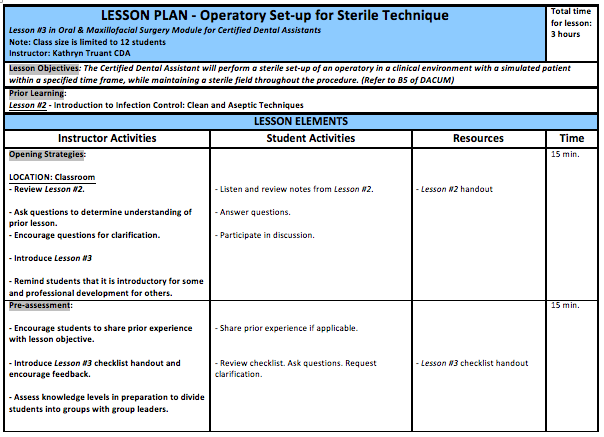
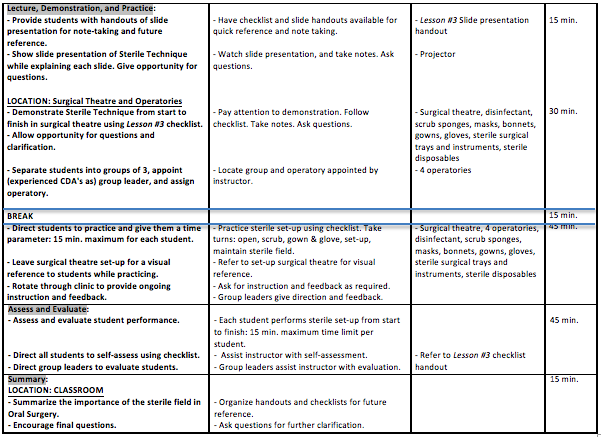
Objective: The Certified Dental Assistant will perform a sterile set-up of an operatory in a clinical environment with a simulated patient within a specified time frame, while maintaining a sterile field throughout the procedure.
While developing my lesson plan, I chose the Seven-Step Process because it is suitable for teaching in the cognitive (why infection prevention is necessary), and psychomotor (how to prevent Oral Surgery associated infections) domains. Once the objective of performing a sterile set-up for an operatory is made clear to students, and a review of any previous lesson as it pertains to this particular lesson plan was discussed, instructional time was allotted for lecture, but the bulk of instructional time was spent on demonstration, practice and assessment. I also found the Seven-Step Process easy to modify in order to support the type of instruction required, because it is better suited for meeting the strict objectives in the specialty of Oral and Maxillofacial Surgery (OMS). For example, my lesson plan does not require debate, brainstorming, decisional activities or much reflection; its purpose is to provide training specific to a vocation.
Reasons for my choices related to the instructor and learner activities, timing, resources, and other key elements in my lesson plan:
I started by researching The College of Dental Surgeons of BC’s (CDSBC) Infection Control Guidelines. The CDSBC provide links and resources on their website on infection prevention, and Dental Assistants are taught the basics of infection prevention in accredited certificate programs, but it is not taught in the depth required for an OMS specialty. Therefore, an advanced and specialty specific lesson needs to exist. Infection control is part of patient and clinic safety, and is one of the most important aspects of Oral Surgery.
Lesson #3 requires a large amount of lesson time (3 hours). I fact, it requires the most lesson time in a module for dental assistants working in OMS because it pertains to every aspect of the practice. Failure to operate a sterile field will delay treatment, but most importantly, a breakdown in basic to advanced infection control techniques will increase the likelihood of an infection occurring from the procedure itself.
Instructing this lesson for 45 minutes in the classroom, and encouraging feedback from the students helps the instructor to pre-assess. The majority of the lesson takes place in a real clinic (with a simulated patient) allowing time for the instructor to demonstrate, and (following a short break), the student to practice and perform. Using actual resources and instrumentation that the students can apply to real-life situations is crucial as well. For example, the students will not pretend to scrub, glove and gown, they will actually be doing it. Creating checklists is also very important to organizing and maintaining a sterile technique; quality control is easy to achieve with the use of a reference that the student can take with them into real-life situations. In addition, the instructor sanctions students who have prior knowledge and experience to share their abilities. Group leaders demonstrate and teach and learn from each other, and from the instructor.
How the activities of this lesson will promote a positive learning environment:
Lesson #3 was designed to reflect a positive learning environment.Supplying the students with all of the references and resources that they will need during the lesson, and that they can take with them, provides ownership of the lesson. Fostering feedback from the students helps the instructor to pre-assess and reinforce that it is okay if some students are new to Oral Surgery while others have experience, and also enables the learner to ask questions.
Give sufficient time for practice, and use the errors that are made during the demonstration, practice, and evaluation portion of the lesson as learning moments; an instructor can positively reinforce and highlight why procedures need to be performed in a specific manner. Having students take turns during the lesson means that they receive immediate feedback from their peers and instructor too. Promoting and encouraging students to self-assess and assess their peers builds confidence. Self-assessment creates a real learning experience that is remembered by the learner.
Checklists are imperative for a positive learning environment – they remove stress from the learning environment by providing key information; that way the learner will not feel pressure to memorize all the information and direction during the lesson. In my experience, real learning occurs when a student can learn in real time, for self-study and for future reference. Checklists promote lifelong learning because all lists need to be updated as procedural requirements advance. I use checklists every day to ensure that all the components of a procedure are in place, thus reducing my own stress! It is important to note that following the lesson; the learner will have to perform the procedure in a real clinical environment to ensure the safety of the patient and the operators.
Summary:
Infection prevention is a critical component of OMS. A lesson plan must be consistent and logical so that real learning takes place in a precise and exact vocation like OMS. The Seven-Step Process was instrumental in outlining Lesson #3, while allowing me to foster a positive learning environment.
My Lesson Plan is clear to me, but I realize that I need to be completely explicit in my lesson planning for another instructor to follow it. And while it is fresh in my mind, it also must make sense to me 6 months from now!
A Lesson Plan, like a Course Profile (DACUM), and a Course Outline needs to follow a logical order, needs to provide detailed information, and needs to be clear to all participants to foster a positive learning environment.

You must be logged in to post a comment.